If you are managing an Achilles rupture and considering treatment options, be informed about the role Prednisone can play. Prednisone, a corticosteroid, is often prescribed for its anti-inflammatory properties. However, its use can be a double-edged sword in the recovery process from tendon injuries.
Research indicates that corticosteroids, including Prednisone, can weaken tendon integrity and potentially increase the risk of rupture. For those recovering from an Achilles injury, understanding this risk is crucial. Instead of relying solely on medication, consider integrating physical therapy for targeted strength training and rehabilitation.
Monitoring your dosage with your healthcare provider can help minimize negative effects while still addressing inflammation. Always communicate openly about your symptoms and any concerns related to your recovery. Adopting a multi-faceted approach to treatment will support a more effective healing process and enhance your long-term mobility.
- Prednisone and Achilles Rupture: A Comprehensive Guide
- Understanding the Risks
- Preventive Measures
- Understanding Achilles Ruptures
- Causes and Risk Factors
- Diagnosis and Treatment Options
- Role of Prednisone in Inflammation Management
- Potential Links Between Prednisone and Achilles Injuries
- Mechanisms of Injury
- Recommendations for Patients
- Dosage Guidelines for Prednisone in Injury Recovery
- Short-term Treatment
- Long-term Use
- Monitoring Side Effects of Prednisone during Recovery
- Rehabilitation Strategies Post-Achilles Rupture
- Consulting Healthcare Professionals about Prednisone Use
- Understanding Dosage and Administration
- Monitoring and Side Effects
Prednisone and Achilles Rupture: A Comprehensive Guide
Patients taking prednisone should closely monitor their tendon health. Research indicates that corticosteroids, including prednisone, may increase the risk of tendon ruptures, particularly in the Achilles tendon. Always consult with healthcare providers before starting or stopping any medication.
Understanding the Risks
Prednisone can lead to weakened connective tissue. This change can heighten the likelihood of injuries, such as Achilles ruptures, especially in individuals who engage in high-impact activities. Be aware of symptoms like pain, swelling, or weakness in the tendon area. If you notice these signs, seek medical attention promptly.
Preventive Measures
Staying physically active while on prednisone is important, but opt for low-impact exercises to minimize stress on your tendons. Incorporate flexibility and strength training exercises tailored to your fitness level to maintain tendon integrity. Discuss any exercise plans with a healthcare professional to ensure safety.
Incorporate dietary elements that support tendon health, including adequate protein intake and vitamin D. Hydration also plays a significant role in tissue maintenance. Monitor your medication regimen and keep the lines of communication open with your healthcare provider to address any concerns related to prednisone and tendon health.
Understanding Achilles Ruptures
Achilles ruptures require immediate attention. Typically, an individual experiences a sudden pain in the back of the ankle, often described as being struck or kicked. Swelling and bruising occur shortly after, with movement becoming difficult. Early diagnosis is critical for a favorable outcome.
Causes and Risk Factors
Achilles ruptures commonly arise from a combination of overuse, inadequate warm-up, and repetitive strain. Specific activities that contribute include running, jumping, and abrupt changes in direction. Risk factors include age, participation in sports, and certain medications such as prednisone. Individuals are advised to perform proper stretching and strengthening exercises to mitigate risks.
Diagnosis and Treatment Options
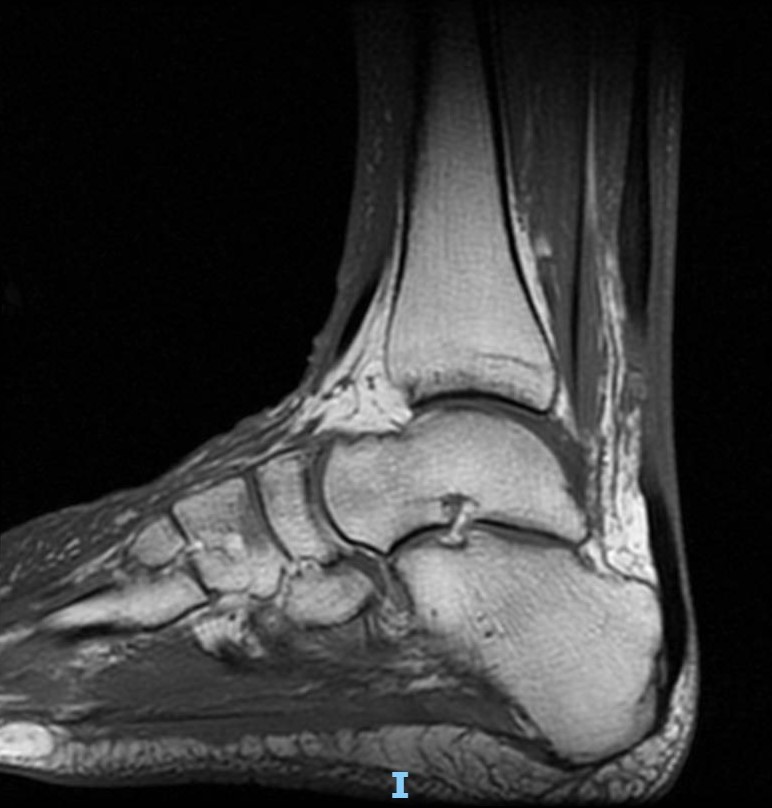
Medical professionals confirm an Achilles rupture through physical examinations and imaging tests like ultrasound or MRI. Treatment typically involves either conservative methods or surgical intervention. For non-surgical treatment, a cast or brace keeps the foot in a pointed position, allowing the tendon to heal naturally. Surgery may be necessary for complete ruptures or active individuals aiming for a full recovery.
| Treatment Method | Pros | Cons |
|---|---|---|
| Conservative | Less invasive, lower risk of complications | Longer recovery time, possible re-rupture |
| Surgical | Quicker recovery, lower re-rupture rate | Higher risk of complications, longer initial downtime |
Physical therapy plays an important role in rehabilitation, focusing on restoring strength, flexibility, and functionality. Patients should engage with healthcare providers to tailor a recovery plan appropriate for their needs.
Role of Prednisone in Inflammation Management
Prednisone serves as a powerful anti-inflammatory agent in the treatment of various conditions, including tendon injuries such as Achilles rupture. By suppressing the immune response, it effectively reduces swelling and pain associated with inflammation. Administering prednisone in the early stages post-injury may facilitate quicker recovery and improved mobility.
It works by inhibiting the production of substances that trigger inflammatory responses. Clinical studies show that prednisone can decrease inflammatory markers, leading to reduced pain levels and enhanced function. Physicians often prescribe it alongside physical therapy to optimize healing outcomes.
Dosage typically starts at a higher level, with gradual tapering based on the patient’s response. Some patients report significant relief within a few days, allowing them to engage more fully in rehabilitation exercises. Monitoring for side effects, such as gastrointestinal issues or increased blood sugar levels, is essential during treatment.
In conclusion, prednisone plays a significant role in managing inflammation, especially for those recovering from an Achilles rupture. Its timely use can promote a faster return to everyday activities and sports, provided the treatment plan includes close supervision by a healthcare professional.
Potential Links Between Prednisone and Achilles Injuries
Research indicates a possible correlation between long-term prednisone use and an increased risk of Achilles tendon injuries. Clinicians must remain vigilant to this association during treatment.
Mechanisms of Injury
Prednisone affects tendon health in several ways:
- Tendon Weakening: Corticosteroids like prednisone can lead to a degradation of collagen synthesis, which weakens the structural integrity of tendons.
- Increased Risk of Rupture: Studies suggest that usage of steroids can lead to changes in tendon morphology, making them more susceptible to rupture under stress.
- Delayed Healing: Prednisone may impair the body’s natural healing processes, prolonging recovery times after injuries.
Recommendations for Patients
For individuals on prednisone, consider the following:
- Discuss alternatives with your healthcare provider if you have a history of tendon injuries.
- Engage in strength training and flexibility exercises to support tendon health.
- Monitor for pain or changes in mobility in the Achilles area and report them immediately.
Maintaining awareness of prednisone’s potential impact on tendons can assist in preventing injuries and ensuring effective management of underlying conditions.
Dosage Guidelines for Prednisone in Injury Recovery
For optimal recovery from injuries such as an Achilles rupture, prednisone dosage typically starts at 20 to 60 mg per day. The exact dose depends on various factors, including the severity of the injury, the individual’s response, and medical history. Gradual tapering is crucial once inflammation stabilizes. A common approach is to reduce the dosage by 5 to 10 mg every week, monitoring the patient’s condition throughout the process.
Short-term Treatment
For short-term use, high doses may be appropriate to manage acute inflammation. Administer prednisone for a period ranging from a few days to several weeks. Consistent follow-up with a healthcare professional allows for adjustments based on recovery progress and side effects.
Long-term Use
For prolonged recovery phases, lower doses between 5 to 20 mg may suffice. Regular assessments help evaluate the necessity of continuing treatment or further adjustments. Always take prednisone with food to minimize gastrointestinal irritation and ensurehydric intake is maintained.
Monitoring Side Effects of Prednisone during Recovery
Regularly assess your response to prednisone. Notice any changes in mood, weight, or appetite, as these can indicate potential side effects. Document daily fluctuations to identify patterns and triggers.
Check your blood pressure frequently. Prednisone may raise it, putting additional stress on your system. If readings consistently exceed normal limits, consult your healthcare provider for adjustments.
Pay attention to gastrointestinal symptoms. Nausea, heartburn, or changes in bowel habits can occur. Discuss any persistent discomfort with your doctor to explore dietary adjustments or medications that might help.
Monitor for signs of infection, such as fever or unexplained fatigue. Prednisone can weaken your immune response, making you more susceptible to illness. Seek medical advice if you experience these symptoms.
Stay hydrated and maintain a balanced diet. Proper nutrition supports your recovery and helps mitigate some side effects like weight gain and mood swings. Incorporate plenty of fruits, vegetables, and lean proteins.
Engage in light physical activity as tolerated, but don’t overexert yourself. Gentle exercises promote circulation and reduce stiffness while keeping an eye on how your body feels during and afterward.
Finally, maintain open communication with your healthcare provider throughout your recovery. Share any concerns or unusual symptoms promptly, allowing for timely adjustments to your treatment plan.
Rehabilitation Strategies Post-Achilles Rupture
Begin rehabilitation with a focus on range of motion (ROM) exercises. Gradually introduce dorsiflexion and plantarflexion movements. Aim for 10 to 15 repetitions, three times a day. Use a towel to assist with stretching, holding each stretch for 15 to 30 seconds.
- Week 1-2: Emphasize gentle ROM and non-weight bearing exercises. Consider using a stationary bike if comfortable.
- Week 3-4: Transition into partial weight bearing. Perform heel slides and ankle alphabet exercises to maintain mobility.
- Week 5-6: Begin strengthening. Incorporate resistance bands for plantarflexion and dorsiflexion exercises. Aim for 3 sets of 10 repetitions.
Integrate balance training after the initial 6 weeks. Use a balance board or perform single-leg stands to enhance stability. Gradually increase difficulty by closing eyes or standing on an unstable surface.
- Balance Training: Start with 15 seconds on a stable surface, progressing to 30 seconds on an unstable surface.
- Strengthening: Include calf raises after the 8-week mark. Start with body weight, then add resistance as strength improves.
- Functional Movements: Introduce walking, then light jogging around 3 months post-injury if cleared by a specialist.
Monitor pain levels and adjust intensity accordingly. Incorporate ice therapy after workouts to manage swelling. Maintain open communication with healthcare providers to ensure optimal recovery.
Lastly, consider the psychological aspect of rehabilitation. Engage in visualization techniques to positively influence recovery and maintain motivation.
Consulting Healthcare Professionals about Prednisone Use
Always approach your healthcare provider before starting prednisone. Discuss any existing medical conditions, current medications, and any potential interactions. Make sure to provide a complete medical history, including allergies and previous reactions to corticosteroids.
Understanding Dosage and Administration
Request clear guidance on the proper dosage tailored to your specific situation. Different conditions may require varying doses. Ask about the timing of medication to ensure it fits well with your routine. Clarify any instructions regarding whether to take the medication with food or on an empty stomach.
Monitoring and Side Effects
Engage in an open dialogue about possible side effects. Discuss what symptoms to monitor and when to seek additional help. Regular follow-up appointments can provide an opportunity to adjust dosage or address any concerns. Always report unusual symptoms such as mood changes, increased appetite, or gastrointestinal issues.